Can Meningitis Be Prevented with Vaccines?
Yes meningitis can often be prevented with vaccines, particularly when the disease is caused by specific bacteria. While not all forms of meningitis are vaccine-preventable, modern immunization programs have significantly reduced the global burden of bacterial meningitis, which is the most severe and life-threatening type.
Understanding Meningitis
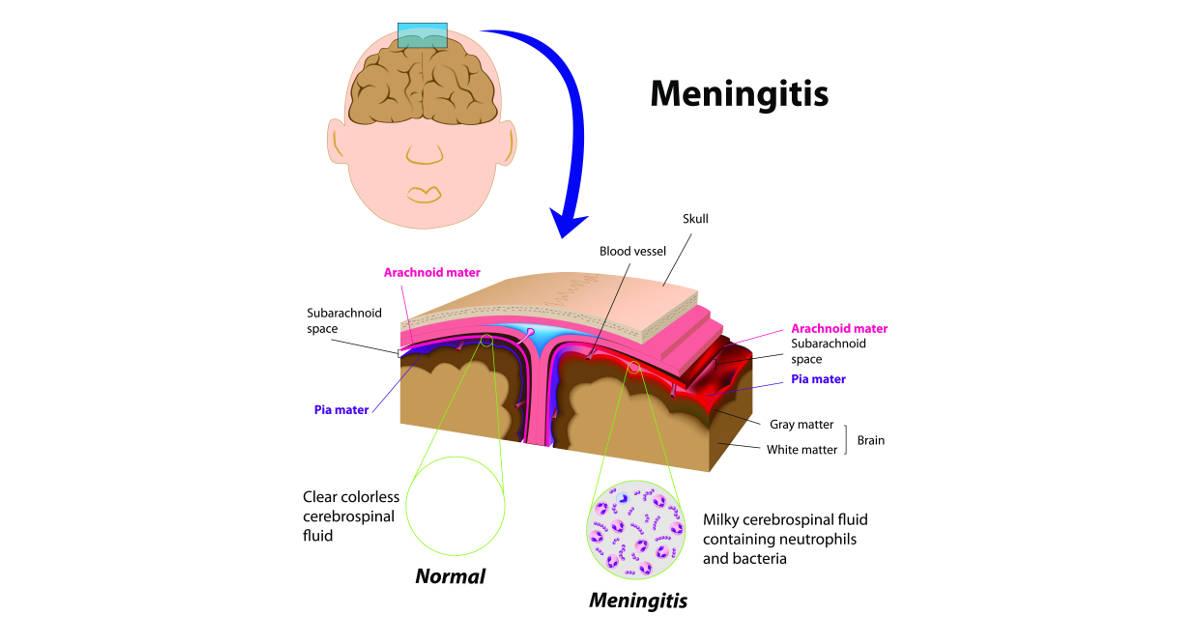
Meningitis is an inflammation of the meninges the protective membranes covering the brain and spinal cord. It can be caused by bacteria, viruses, fungi, or parasites. The most dangerous form is acute bacterial meningitis, which can lead to brain damage, hearing loss, septicemia, or death if not treated promptly.
Among bacterial causes, the most clinically significant pathogens include
-
Neisseria meningitidis
-
Streptococcus pneumoniae
-
Haemophilus influenzae type b
Vaccination strategies target these organisms specifically because they account for the majority of severe bacterial meningitis cases worldwide.
Which Vaccines Prevent Meningitis?
1. Meningococcal Vaccines
Vaccines against Neisseria meningitidis protect against several serogroups (A, B, C, W, Y). These vaccines are commonly recommended for
-
Adolescents and young adults
-
College students in dormitories
-
Military recruits
-
Travelers to endemic regions (e.g., sub-Saharan Africa’s meningitis belt)
-
Individuals with complement deficiencies
Routine vaccination programs have dramatically reduced meningococcal disease incidence in many countries.
2. Pneumococcal Vaccines
Streptococcus pneumoniae is a leading cause of meningitis in infants, older adults, and immunocompromised individuals.
Two main vaccine types are used
-
Pneumococcal conjugate vaccines (PCV)
-
Pneumococcal polysaccharide vaccines (PPSV)
Widespread use in childhood immunization schedules has not only protected vaccinated individuals but also contributed to herd immunity.
3. Hib Vaccine
Before routine immunization, Haemophilus influenzae type b was the most common cause of bacterial meningitis in young children.
The introduction of the Hib vaccine led to a dramatic decline over 95% reduction in many developed countries. It remains a core component of pediatric vaccination programs worldwide.
How Vaccines Prevent Meningitis
Vaccines stimulate the immune system to produce antibodies against specific bacterial antigens. If exposed later, the immune system recognizes and neutralizes the pathogen before it invades the bloodstream and crosses the blood-brain barrier.
This prevention mechanism interrupts two critical steps in meningitis pathogenesis
-
Nasopharyngeal colonization
-
Hematogenous spread to the central nervous system
By reducing colonization rates, vaccines also decrease transmission in the community, providing indirect protection (herd immunity).
Limitations of Vaccination
Although vaccines significantly reduce bacterial meningitis, they do not prevent
-
Viral meningitis (most commonly caused by enteroviruses)
-
Fungal meningitis (e.g., in immunocompromised patients)
-
Rare bacterial strains not included in vaccine formulations
Additionally, vaccine coverage gaps, supply chain challenges, and regional disparities still allow outbreaks to occur.
This is where treatment infrastructure becomes crucial including reliable access to antibiotics through established ceftriaxone injection supplier channels.
The Role of Ceftriaxone in Meningitis Management
Even with strong vaccination programs, meningitis cases still occur. When bacterial meningitis is suspected, empiric intravenous antibiotics must be administered immediately, often before laboratory confirmation.
One of the cornerstone treatments is ceftriaxone, a third-generation cephalosporin with
-
Broad-spectrum gram-negative coverage
-
Good cerebrospinal fluid (CSF) penetration
-
Proven efficacy against meningococcus and pneumococcus
In many healthcare systems especially in low- and middle-income countries timely access depends on dependable procurement networks and partnerships with a trusted ceftriaxone injection supplier.
During meningococcal outbreaks, public health authorities often stockpile ceftriaxone to ensure rapid mass treatment capability.
Vaccination vs. Treatment: Why Prevention is Superior
While ceftriaxone and other antibiotics save lives, treatment has limitations
-
Mortality remains 5–15% even with therapy
-
Survivors may experience neurological sequelae
-
Delays in treatment significantly worsen outcomes
Vaccination eliminates these risks by preventing disease onset altogether.
Moreover, over-reliance on antibiotics increases antimicrobial resistance risk. Preventive immunization reduces antibiotic demand and preserves drug efficacy.
Global Impact of Meningitis Vaccines
The introduction of meningococcal conjugate vaccines in Africa’s meningitis belt has reduced serogroup A epidemics by over 99% in vaccinated populations.
Similarly
-
Hib vaccination virtually eliminated pediatric Hib meningitis in high-coverage countries.
-
Pneumococcal vaccination significantly reduced invasive pneumococcal disease rates.
These achievements demonstrate that meningitis prevention is not theoretical it is a documented public health success.
Who Should Get Vaccinated?
Recommendations vary by country, but generally include
-
Infants (Hib and pneumococcal series)
-
Adolescents (meningococcal vaccines)
-
Adults over 65 (pneumococcal vaccines)
-
Immunocompromised individuals
-
Travelers to endemic areas
Healthcare providers assess risk factors including age, comorbidities, geographic exposure, and institutional living conditions.
Future Directions in Meningitis Prevention
Ongoing research aims to
-
Expand serogroup coverage
-
Improve long-term immunity
-
Develop broader pneumococcal vaccines
-
Enhance global vaccine accessibility
Simultaneously, strengthening pharmaceutical supply chains remains vital. In outbreak scenarios, coordination between vaccination campaigns and antibiotic distribution often through established ceftriaxone injection supplier systems ensures both prevention and rapid response capacity.
Conclusion
Yes, meningitis can be prevented with vaccines particularly bacterial meningitis caused by meningococcus, pneumococcus, and Hib. Immunization has dramatically reduced incidence, mortality, and long-term complications worldwide.
However, vaccination does not eliminate all cases. When bacterial meningitis occurs, immediate antibiotic therapy often with ceftriaxone is lifesaving. Reliable access to treatment through a dependable ceftriaxone injection supplier remains a critical component of healthcare preparedness.
Ultimately, the most effective strategy combines
-
High vaccination coverage
-
Rapid diagnosis
-
Immediate antibiotic treatment
-
Strong pharmaceutical supply infrastructure
Prevention through vaccination remains the safest, most cost-effective, and most impactful method to combat meningitis globally.
- SEO
- Biografi
- Sanat
- Bilim
- Firma
- Teknoloji
- Eğitim
- Film
- Spor
- Yemek
- Oyun
- Botanik
- Sağlık
- Ev
- Finans
- Kariyer
- Tanıtım
- Diğer
- Eğlence
- Otomotiv
- E-Ticaret
- Spor
- Yazılım
- Haber
- Hobi
